The Worst Advice You'll Get About Joint Pain (And What To Do Instead)
My client had been dealing with knee pain on stairs for months. She finally went to see a physical therapist. He assessed her, gave her some stretches, and told her to stop lifting weights.
She pushed back. "It doesn't hurt when I lift, and I have an online trainer checking my form. Why would I stop?"
He told her to stop anyway.
When she relayed this to me, I had to bite my tongue. I don't like to bash other PTs, but that was the worst possible advice he could've given her.
Because the fastest way to make a painful joint worse is to stop loading it.
Why Strength Training Is The Key To Feeling Better
The thing that so many people (and some PTs) get wrong is that pain doesn't always mean damage.
And avoiding load doesn't fix the problem. In most cases, it makes it worse.
When you stop lifting, you lose muscle.
When you lose muscle, your joints absorb more force.
When your joints absorb more force with less muscular support, they hurt more.
You get weaker, and things that used to feel fine start to feel hard.
So you do less, and the vicious cycle accelerates.
This is how a manageable knee issue at 45 becomes a knee replacement conversation at 60.
Your muscles, tendons, cartilage, and bone adapt to the demands you place on them. Load them progressively and they get stronger. Remove the load and they shrink. And once that happens, the activities you care about start slipping away — hiking, skiing, golf, even walking down the stairs without holding the railing
That's often when they come to see me in the PT clinic.
But strength training is one of the most effective interventions we have for reducing joint pain. And that's not my opinion, the research is overwhelming:
A 2015 Cochrane Review — the gold standard for evidence synthesis — pooled data from 54 randomized controlled trials and found that exercise reduced knee osteoarthritis pain by about 12 points on a 100-point scale and improved physical function by 10 points. That effect size is comparable to taking NSAIDs, except exercise doesn’t stop working after you swallow the last pill.
Even more striking: a randomized controlled trial published in the New England Journal of Medicine took 100 patients with moderate-to-severe knee osteoarthritis who were eligible for total knee replacement and split them into two groups — one got surgery plus rehab, the other got a 12-week nonsurgical program of exercise, education, and dietary guidance. Of the 50 patients in the nonsurgical group, 74% never needed the surgery. These were people who qualified for a knee replacement, did structured exercise instead, and three out of four of them were fine.
And if you're someone who's been told to skip PT and just get a cortisone shot, consider this: a 2020 trial, also in the New England Journal of Medicine, compared physical therapy to glucocorticoid injections for knee osteoarthritis. At one year, the PT group had better outcomes. The thing most people reach for first — the quick injection — performed worse long-term than the thing most people skip.
The answer to pain is almost never "do less and rest." It's "do the right things, in the right way, and build back the capacity your body has lost."
Free Download
The Pain-Free Loading Guide
Starter exercises for knee, back, and shoulder pain — plus the framework for knowing when to push and when to pull back.
Why The Envelope Of Function Is The Most Important Rehab Concept You've Never Heard Of
At Duke, I learned from some of the best minds in physical therapy.
One of them was Dr. Michael Reiman, a world-renowned orthopaedic PT specialist. In his class, he introduced a concept originally developed by orthopedic surgeon Dr. Scott Dye called the "Envelope of Function."
When I first heard it six years ago, I thought: "Duh! Doesn't everyone already know this?" It seemed obvious.
But after 3.5 years of practicing, I realized that almost nobody — patients, trainers, even many PTs — actually thinks about injury this way. And it's the single most useful framework I've ever encountered for understanding why you hurt and what to do about it.
Here's the idea:
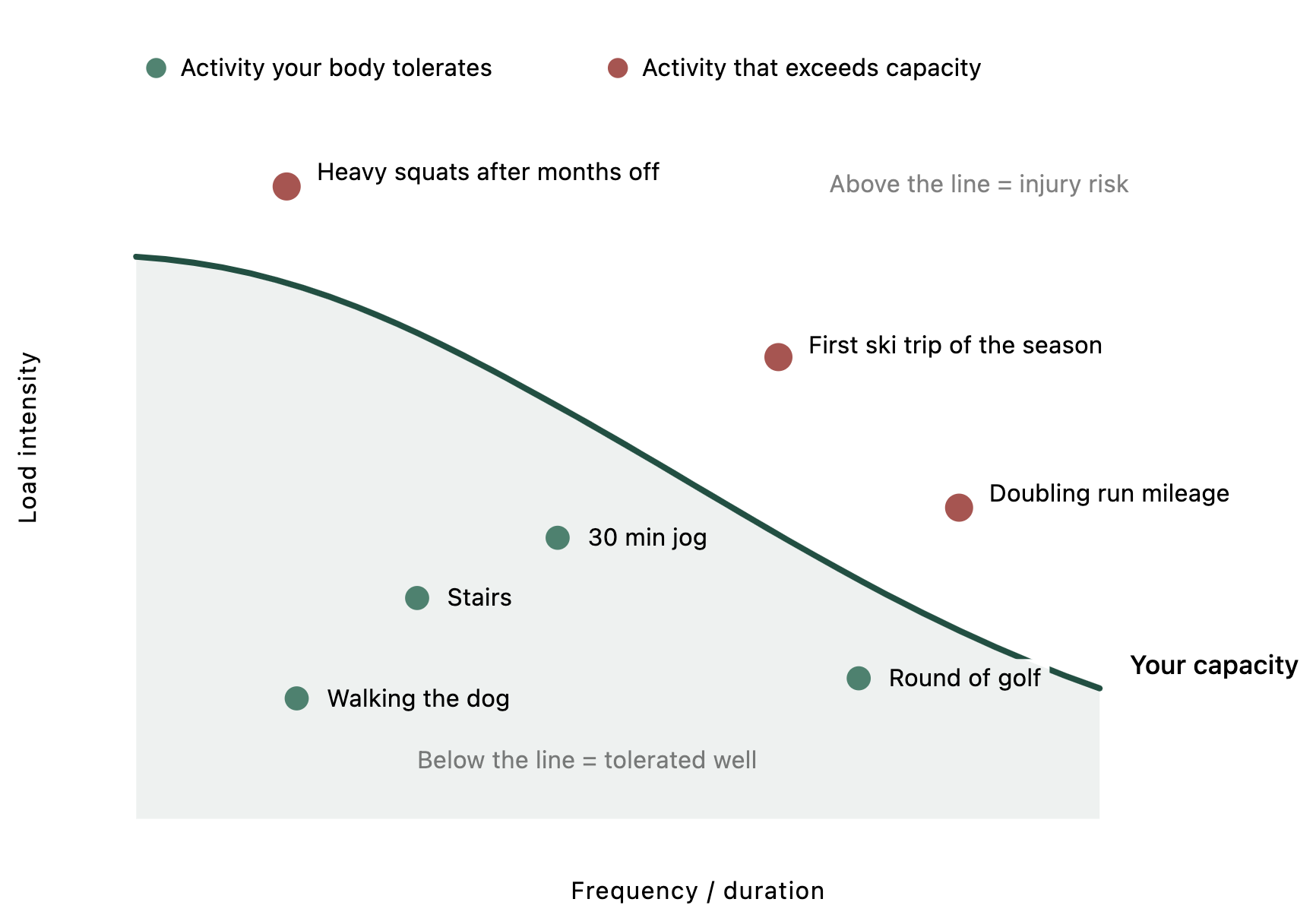
Every tissue in your body — your muscles, tendons, cartilage, bones — has a capacity. Think of it as a threshold line. Below that line, you can do things without pain. Walk the dog, go for a hike, squat in the gym, play 18 holes. Your body tolerates it and recovers. That range of activities you can handle comfortably is your envelope of function.
The critical thing to understand is that this line is not fixed. It moves up and down based on your life.
Sleep poorly for a week and that capacity line drops.
Pile on stress from work or a bad stretch at home and it drops further.
Stop training for a few months and it drops a lot
On the other side, stay consistent with smart training, sleep well, manage stress, eat enough protein, and that line rises. Your envelope expands. You can handle more before your body starts complaining.
Injury happens when the demands you place on a tissue exceed its current capacity. You go on a ski trip after not training all winter. You jump back into heavy squats after three months off. You ramp up your running mileage too fast during a stressful period at work when you're sleeping five hours a night. The demand crosses the line, and the tissue can't adapt fast enough.
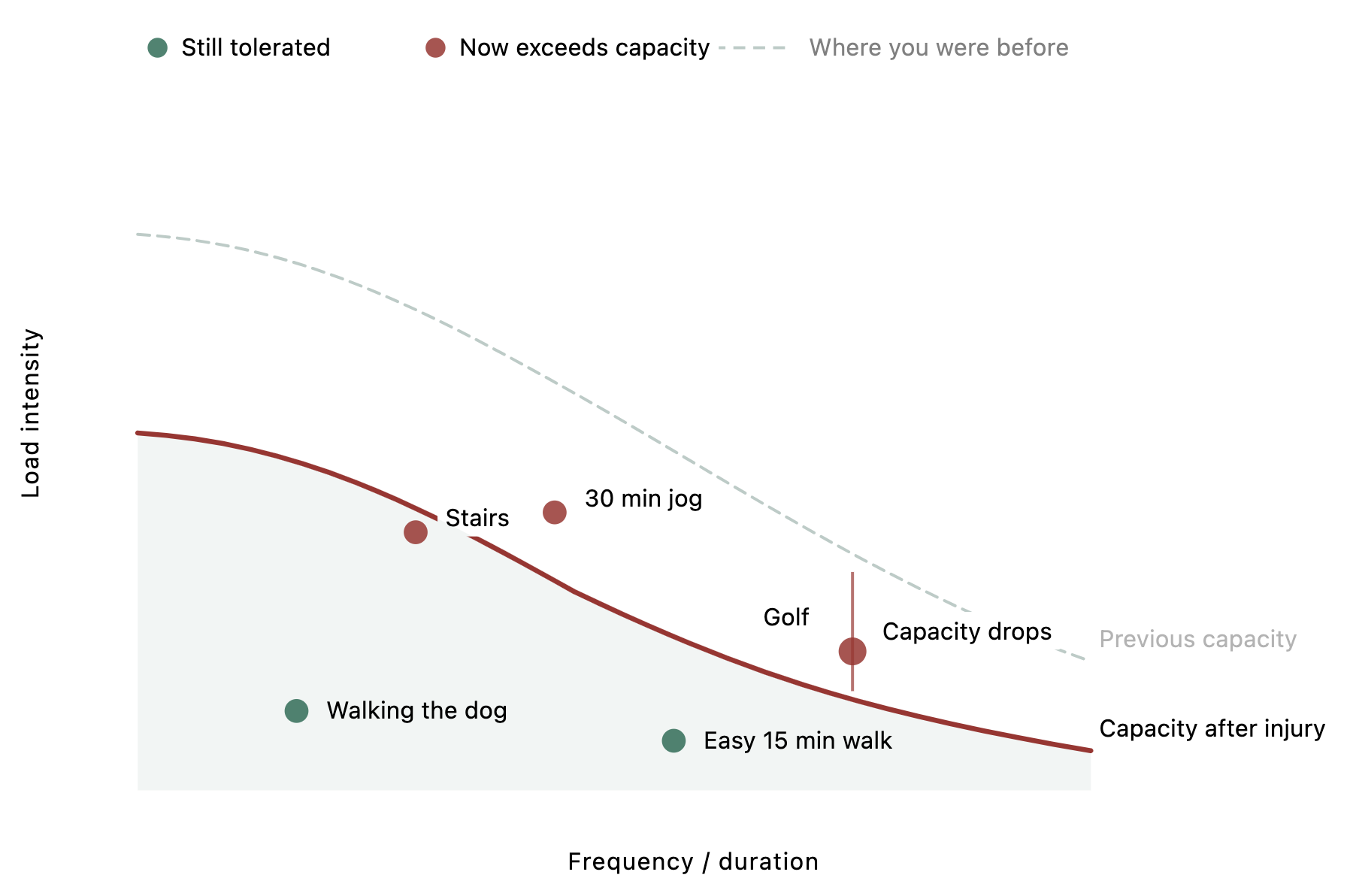
And here's the key: once you get injured, your capacity drops even further. The line falls.
Activities you could tolerate last month are now too much. So you do less, which makes you weaker, which drops the line again. This is the exact vicious cycle I described earlier, and the envelope of function gives you a visual framework for understanding why it happens.
The good news? The process works in reverse, too.
How To Expand Your Capacity
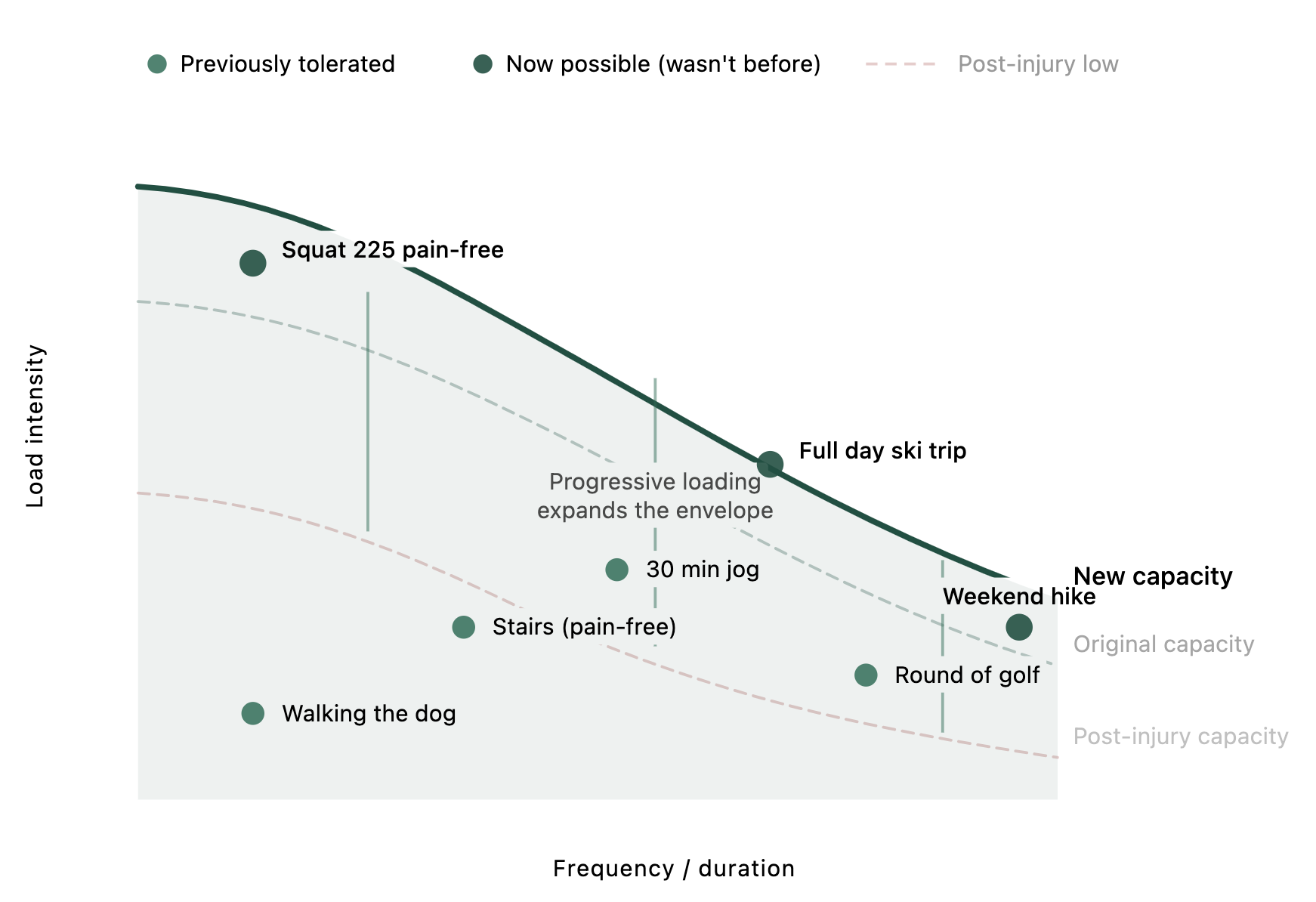
Once you find the activities your body can currently tolerate — even if that starting point is humbling — you have a baseline. From there, you progressively increase the demand, just enough to challenge the tissue without blowing past its capacity.
The tissue adapts, the line rises, and our envelope grows. And over time, activities that used to cause pain don't anymore, because your capacity has expanded past the point where those demands are a problem.
That's what good rehab actually is!
It's not resting until the pain goes away and hoping it doesn't come back. It’s not cramming pain pills down your gullet or masking your symptoms with injections. The entire game is finding where your capacity currently sits, respecting that starting point, and systematically building it back up until your envelope is bigger than it was before you got hurt.
This is the concept behind every program I write, every progression I make, and every decision about when to push harder and when to pull back. The envelope of function isn't complicated, but applying it correctly — knowing how hard to push, when to modify, and how fast to progress — is where most people need help.
I saw this meme from @dr.dave.strengthandkindness the other day and it perfectly encapsulates this idea:
What actually moves the line?
Here are the five things that actually expand your envelope and reduce pain over time
Progressive overload through training. This is the biggest lever.
Strength training builds muscular and connective tissue capacity that protects your joints.
Mobility work expands accessible range of motion.
Cardiovascular training improves your aerobic base so sustained activities don't push you past the line.
And activity-specific training prepares your body for the exact demands you care about — if you want to ski without your knees screaming, you need to train movements that mimic the forces skiing puts on your body. Generalized fitness helps, but specific preparation is what closes the gap.
Nutrition and hydration. Your tissues can't rebuild what you don't give them the raw materials for. Adequate protein — roughly 0.8 to 1 gram per pound of lean body mass — supports muscle repair and tendon remodeling. Staying well hydrated keeps your cartilage, discs, and connective tissue functioning the way they're designed to. And a diet built around whole, nutrient-dense foods gives your body the micronutrients it needs to recover.
Sleep. This is when the majority of tissue repair happens. If you're training hard but sleeping five or six hours a night, you're writing checks your recovery can't cash.
Stress management. Chronic stress elevates cortisol, impairs recovery, increases pain sensitivity, and lowers your tolerance to physical demand. It may seem strange that what goes on inside your head impacts your body but, trust me, unchecked stress directly lowers the capacity line.
Avoiding setbacks. Expanding the envelope requires staying just below the line consistently, not blowing past it every few weeks and crashing back down. Every major setback costs you weeks of rebuilding. The fastest way to expand the envelope is, paradoxically, to be patient enough to stay inside it while you push its edges.
What Won't Move The Line (Much)
Here's where people waste enormous amounts of time and money:
Ice baths, saunas, cryotherapy, red light therapy — these might feel good, but they don't build capacity. They don't make your tendons stronger or your joints more resilient. At best, they support your ability to train. At worst, they're expensive distractions that give you the feeling of progress while the needle doesn't move.
Pain pills and cortisone injections mask symptoms. They can be useful in specific situations — calming an acute flare-up so you can get back to loading, or creating a window where rehab is tolerable. But they don't fix anything. The tissue is still weak. You just can't feel it, which is how people re-injure themselves doing something they thought they'd recovered from.
Passive rest is the strategy most people default to. And for acute injuries, a brief period of relative rest makes sense. But beyond that initial phase, rest alone doesn't restore capacity.
Peptides, supplements, and whatever the latest biohacking trend is — some are helpful in specific contexts. But none of them replace the fundamentals. No peptide builds the quad strength that protects your knee. If your training, nutrition, sleep, and stress management aren't dialed in, stacking supplements on top is like putting premium gas in a car with flat tires.
What This Looks Like In Practice
You're probably wondering what this actually looks like when someone applies it. Here are two examples.
Important caveat: the specific exercises, timelines, and loading progressions below are all illustrative. Every injury is different, and yours would need to be tailored to your body, your history, and your starting point. But the framework — find the floor, build capacity, bridge to the goal, expand past where you were — applies to nearly everyone.
Getting Back To A 3-Mile Run After Patellar Tendonitis
You used to run three miles a few times a week without thinking about it. But last week your knee started barking — right below the kneecap, worse going downhill, worse the morning after a run. You pushed through it because you're an athlete. Now it hurts walking down stairs and running is off the table.
Your envelope just shrank. Don't panic.
Here's how you build back:
Weeks 1–2: Find the floor. Can you walk 20 minutes without a flare-up the next day? Can you do bodyweight squats to a comfortable depth? Isometric wall sits for 30–45 seconds? You're looking for the activities your tendon currently tolerates. That's your new baseline.
Weeks 3–6: Build tendon capacity. Heavy slow resistance training — leg press, Spanish squats, single-leg decline squats — loaded progressively, 3–4 sets of 8–15 reps, 3x per week. Start walk/jog intervals (4 min walking, 1 min jogging) and monitor response over 24 hours.
Weeks 7–9: Bridge to running. Intervals shift toward more jogging, less walking. Remember, the tendon capacity you're building in the gym is what allows the running to be tolerated. So, keep strength training!
Weeks 10–12: Expand the envelope past where it was. Add distance slowly, no more than 10–15% per week. By week 12, you're back to three miles with a tendon that's stronger than before the injury.
Getting Back To A 225 Back Squat After A Low Back Strain
You tweaked your back pulling a heavy deadlift. Tying your shoes was an event, sitting for 20 minutes was miserable, and you haven't touched a barbell in six weeks.
Come on, we’ve been over this! Don’t panic.
Your envelope for spinal loading is way down. How to get it back up:
Weeks 1–3: Find what you can do. Goblet squats with a 25-pound dumbbell, glute bridges, side planks. Stay active, keep the muscles around the spine engaged, and avoid the deconditioning spiral.
Weeks 4–6: Rebuild spinal loading tolerance. Goblet squats get heavier. Add trap bar deadlifts focusing on bracing mechanics. Front squat before back squatting — the upright torso places less shear on the lumbar spine. Monitor how your back responds in the 24 hours after training.
Weeks 7–9: Return to the barbell. Start at 95 or 135. Movement pattern should feel solid before the weight gets ambitious. Sets of 5–8, adding 5–10 pounds per week as tolerated.
Weeks 10-12+: Expand past your old capacity. By now you're squatting in the 185–205 range and your back feels better than it did before the strain.
The key in both examples: at no point did the answer involve stopping entirely and waiting.
The answer was finding the right starting point, loading progressively, and being patient enough to let the tissue adapt.
Free Download
Ready to Start Loading?
The Pain-Free Loading Guide has the exercises, self-assessment, and pain monitoring framework to get you started today.
If You're Dealing With Pain
If you have pain, bookmark this article. If you know someone in pain, send it to them.
Your body is resilient and you will get out of pain. But it takes patience and an unwavering commitment to the principles in this article.
And if you'd like a partner along the way to getting back to full strength, I help people with this every day. Schedule a free call, and let’s get you feeling better fast:
Best,
John
P.S. My Duke girls!
3 Steps You Can Take
Apply for coaching - If you’re ready to start, you can fill out a coaching application here (it takes 90 seconds or less). Best case, you change your life. Worst case, I’ll help you draw up a road map to get closer to your goals.
Sign up for my newsletter - If you’d like to hear more, sign up for my mailing list here.
Keep learning - You can check out my other articles here. Nobody asked me to, but I’ve spent a ton of time researching everything from artificial sweeteners to saturated fat to testosterone and more, so you don’t have to.




![Diagram comparing what actually moves the capacity line (progressive overload, nutrition, sleep, stress management) versus what doesn't move it much (ice baths, pain pills, passive rest, supplements)]](https://images.squarespace-cdn.com/content/v1/5e727e25d12f642e2a05bd8d/0e9c67ff-fa8f-49ff-a9c1-de22b27f452d/Screen+Shot+2026-03-21+at+11.12.40+AM.png)


